EECP® Therapy Patient Preparation
Pre-Treatment Instructions
Pretreatment Evaluation
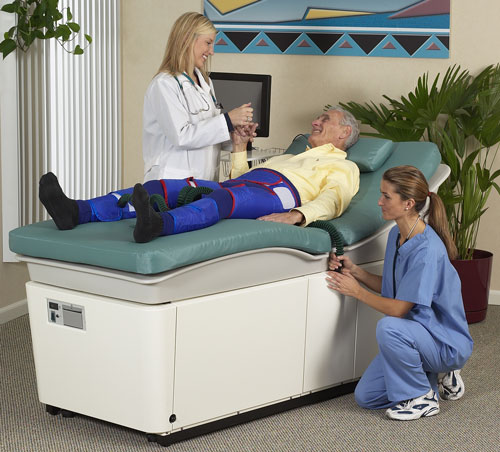
Careful review of the patient's medical history and current medical status before beginning treatment will contribute to a safe treatment experience and a positive therapeutic outcome. A complete physician evaluation of a prospective patient (including physical examination, medical history and twelve lead ECG) will assist in determining a patient's eligibility for EECP® Therapy treatment.
A recent history and physical (within 3 months) and a recent ECG (within one month) are useful in qualifying the patient for treatment, particularly when the patient is referred by a physician other than the medical director of the EECP® Therapy center.
Cardiac catheterization intervention reports, open heart and/or CABG operative reports, stress test, vascular study, echocardiography and nuclear study reports as well as a complete list of current medications, and recent laboratory reports are important components of a thorough pre-EECP® Therapy patient evaluation.
Diagnostic evaluation may include: Twelve lead electrocardiogram (ECG), x-ray, exercise stress test (ETT), echocardiography and coronary angiography.
Further tests may include doppler studies or arterio venograms of the lower extremities for assessment of peripheral vascular disease (PVD) or thromboembolus. For some patients an abdominal ultrasound may be performed for assessment of abdominal aortic aneurysm. A pregnancy test is important for women of childbearing age, as are periodic INR tests for patients treated with anticoagulants.
Current experience indicates that EECP® Therapy presents minimal risk with careful patient selection. Nevertheless, prior to receiving EECP® Therapy, patients should be evaluated in keeping with the standards of good medical practice.
Pretreatment Patient Preparation
It is best if patients are stabilized for two weeks prior to initiating treatment. Fluid volume status must be well managed. Patients should be treated with medications until a euvolemic state is achieved. Control of symptoms while maintaining the patient's medication regimen at a "steady state" is a good indicator that the patient's condition has stabilized.
A physician evaluation performed immediately prior to the start of therapy assessing the patient's fluid volume status helps to ensure that the patient is stable and ready to begin EECP® Therapy.
To support safe and effective treatment, the EECP® Therapist maintains communication with the prescribing physician and/or EECP® Therapy medical director. Physician evaluation and management should be ongoing as the patient progresses through therapy and as required should include:
- Regulation of medications
- Management of fluid volume status
In the event of an exacerbation of congestive heart failure symptoms, EECP® treatment should be withheld. Treatment may be resumed when in the physician's opinion the patient's condition has been stabilized.
Dosage Protocol
A usual course of EECP® Therapy consists of 35 hours of treatment:
- One hour per day, five days per week for a seven week period
- Alternatively, patients may be treated one hour per day for the first five days of treatment. If tolerated, the patient may then receive two one-hour treatments per day separated by at least a 30 minute break, for the following four weeks. This treatment regimen is typically reserved for patients traveling long distances or with personal time constraints.
Treatment dosage is based upon achievement of therapeutic objectives. For patients with angina, decreased episodes of angina with increased exercise tolerance are measures of progress. In some patients the effectiveness of EECP® Therapy may be limited by physical factors, degree of morbidity and comorbidities. Additional hours of therapy may be considered to achieve treatment objectives.
It is important that patients accepted for EECP® treatment be prepared to comply with the treatment regimen as prescribed by the physician; continuity of treatment is important to a successful outcome. Missed treatment hours (excluding weekends) should be added to complete the 35 hour requirement. Patient commitment to therapy is essential.
Patient Education
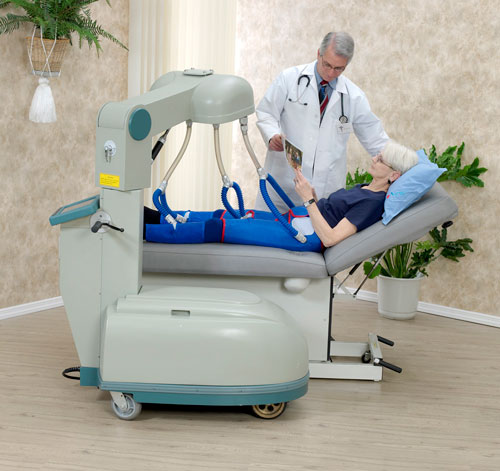
Education is key to pretreatment patient preparation. Medical care may cause anxiety in many patients and a thorough explanation of treatment may alleviate a patient's fears. An orientation program during which patients and their families are given literature, videos, DVDs, web site address and are guided to a list of chat rooms to learn about EECP® Therapy and share ideas may be offered. Where possible, and with permission of patients receiving EECP® Therapy, prospective patients should be offered the opportunity to observe treatment and ask questions. Patient support and awareness groups have also been helpful in enhancing awareness and understanding of EECP® Therapy. The Vasomedical, Inc. patient information web site is located at www.naturalbypass.com.
EECP® Therapists play an important role in managing patient expectations. While most patients treated with EECP® Therapy demonstrate improvement, some experience improvement in the early stages of treatment. Other patients may need extended hours of treatment to feel improvement.
Initiating a course of EECP® Therapy may be compared to starting an exercise program. Early in therapy patients may experience fatigue and leg soreness, as is the case with most exercise programs. However, as treatment progresses, the fatigue and soreness typically subside. The patients experience less angina with increased energy and exercise tolerance.
When scheduling the EECP® treatment hour, consideration of the patient's specific dietary and medication regimens is important. The patient will be more comfortable during treatment if no food or fluids are consumed for at least 90 minutes prior to EECP® Therapy.
Juice or other simple sugars should be available as some diabetic patients have experienced hypoglycemia (low blood sugar) post treatment.
All medications should be taken as prescribed. As patients progress through treatment, dosage adjustments may be indicated.
- Patients treated with diuretics should have treatment scheduled for a time when the desired effects of these medications have subsided.
- Patients taking blood pressure medication should be closely monitored.
Record medication changes on the patient's Medication Profile, including the date of the change, the new dose prescribed and the reason for the adjustment. [Unit 7-9 in the The Therapist's Guide to Enhanced External Counterpulsation]
Encourage patients to urinate immediately prior to treatment to minimize interruptions during the treatment hour.
Patient Treatment
Empathy for each patient reflects awareness of their individuality and may serve to promote feelings of comfort and security. The first hour of therapy can set the tone for all that follows. Try to establish an open, supportive relationship with patients encouraging them to discuss fears, discomfort and questions; emphasize the importance of communicating discomfort in order to prevent secondary problems that might interfere with treatment (i.e. skin irritation and breakdown).
Patient Comfort
Encourage patients to relax during therapy. Comfort enhances the effectiveness of EECP® Therapy since greater blood flow is achieved when muscles are relaxed and vascular beds are dilated.
The patient may hesitate to admit to any discomfort for fear that treatment may be terminated. Many patients have exhausted all other treatment options and have invested a great deal of hope in the success of EECP® Therapy. Observe the patient carefully, evaluate emotional status and encourage the patient to relax before beginning treatment (hold the patient's hand, engage in soothing conversation).
Investigate any increase in heart rate, as an increase may signal anxiety, fear, angina, other physical discomfort or the need to urinate. Reassure the patient that interrupting treatment to ease discomfort will not diminish its efficacy, but will actually serve to enhance effectiveness when the patient is again relaxed and comfortable.
Preventing Skin Irritation
Patients should advise the therapist of any pressure, pinching or skin sensitivity during treatment. Treatment may be interrupted, cuffs unwrapped, treatment pants and cuff lining checked for wrinkles or creases. Rewrap cuffs taking care to smooth any wrinkles. If discomfort persists, a piece of lamb’s wool may be used to pad the area. Padding should be limited to areas of focal pressure as excess padding may diminish the effectiveness of compression.
All patients, especially those with diabetes, patients with venous stasis, and those prone to skin breakdown are urged to moisturize their legs with lotion in the evenings, after treatment, and each day immediately before treatment, and to wear tight fitting pantyhose. These measures provide extra protection against skin irritation.
Skin irritation, blistering, ecchymosis or any open lesion requires immediate attention. Irritated skin may appear reddened immediately after treatment and the area may blister or break down during the night. Contact the physician for a treatment order. Do not secure dressings with tape under the cuffs as this may lead to further skin breakdown. Instead, place a gauze pad over the lesion and under the treatment pants. Additional padding over the affected area may be used to prevent further irritation. Encourage the patient to leave the irritated area open to air when at home. If a lesion should occur on the lower legs, treatment may be administered without one or both of the calf cuffs until the skin condition improves. If a lesion is too severe or fails to heal, treatment may have to be suspended.
